About the Hip and Hip Replacement
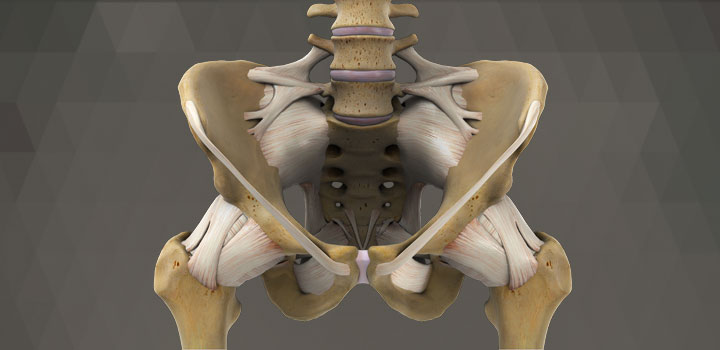
Hip Anatomy
A hip joint consists of two bones – the femoral head (the ball) and the acetabulum (the socket).
Usually the joint is well lubricated and the one bone can slide against the other bone with minimal friction.
However, with diseased hips, the cartilage covering the surface of the bone is worn away and we now have a situation in which the bones are rubbing against each other, causing pain and limiting movement.
Joints can be destroyed for a variety of reasons, but arthritis is the most common.
What is a Hip Replacement?
A Hip Replacement is a surgical procedure — performed in the US since the 1960s — which involves the removal of the diseased or damaged bone joint and the reconstruction of the anatomy with an artificial joint called a prosthesis.
Made of metal alloys and high-grade plastics (which are intended to mimic the function of bone and cartilage, respectively), the prosthesis is designed to move just like a healthy human joint.
There is a femoral stem – a metal component that is placed into the thigh bone, and an acetabular cup – a metal backed component with different options for a liner – plastic, metal and ceramic, that is placed where the socket was.
Over the years, hip replacement techniques and instrumentation have undergone countless improvements. Today, hip replacement is one of the safest and most successful types of major surgery; in well over 90% of cases it is complication-free and results in significant pain relief and restoration of mobility.
There are two goals with Total Hip Replacement:
- Reduce or eliminate pain.
- Restore movement and improve function.
Are You a Candidate for Hip Joint Replacement?
If you and your doctor decide that total hip joint replacement would be advantageous, you should fully understand the risks and benefits of the procedure
An artificial hip joint replaces your natural hip joint with one made of metal and plastic or ceramic that is pressed or cemented into place.
The goal is to relieve pain and improve motion and function. Artificial joints can be very successful in achieving these goals.
The questions that patients most frequently ask is “How long will the replacement last?” The duration of the implant varies depending on your age, activity level and many other factors.
The more demand that is placed on the artificial joint, the greater the potential for wear and failure over time.
Longevity may also be dependent of the type of material used for the artificial joint. There is certainly no consensus as to the best material for the articular surfaces placed in a hip joint. The best choice may depend on the age of the patient and the demand to be placed on the material. Talk to your doctor about the implant options that are best for you.
With your new hip joint replacement, it is ok to walk, bike, golf and play doubles tennis. Ultimately, someone who chooses to undergo hip joint replacement will have to accept some limits in physical activity. It is important for you to talk to your surgeon about your desires and anticipated demands before considering this procedure.
What should you expect?
Blood Transfusion
If you are donating blood for your surgery, you will be asked to donate at least 2 or 3 units of your own blood within 35 days prior to your surgery date. This will involve scheduling an appointment with one of the local Broward Community Blood Centers. Only one unit of blood can be donated at a time, so you will need to come in for at least two visits. The blood is then stored until your operation.
If you are unable to donate blood, for whatever reason, donor blood will be used in your case, if necessary. People have expressed some concern about blood transfusion because of the risk of transmitting diseases. Donor blood is carefully screened for communicable diseases. With the new technology, the risk of hepatitis and HIV infection is extremely low. To our knowledge, disease transmission through use of donated blood has never occurred in any of our patients.
However, there is no question that your own blood is the safest. Therefore, if you are able, we recommend that you donate blood for your surgery. If you’re coming a long way, arrangements can be made to have you give blood locally and have it transported here for your surgery. Please be assured that the blood you give will be given back to you, if needed.
Pre-admission Testing
Within two weeks prior to your surgery, you will be asked to undergo several laboratory tests and possibly an electrocardiogram and chest x-ray. This is called pre-admission testing. This will help us to tell whether there are any conditions which might increase the risk of surgery. A physical examination, performed by your own medical doctor, is also a part of pre-admission testing.